Dear Leader Reid and Speaker Pelosi,
Provisions in the Senate and House health care reform bills propose to reallocate resources based on geographic differences in Medicare spending. While well intended, they will penalize providers who care for the poor and impair access for these vulnerable patients.
A reallocation of resources to lower-cost states has been endorsed by members of Congress from states with lower Medicare spending who believe that, by receiving less from Medicare, their states are currently being penalized for being “efficient.” However, it is not efficiency that accounts for their lower spending. It is less poverty and better health status. 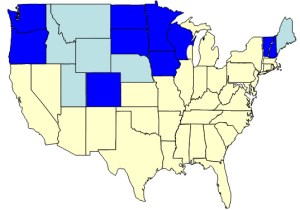
The map shows (in blue) the ten states represented by members of Congress who have publicly endorsed reallocation plans based on geographic differences. Six neighboring states with similar characteristics are lightly shaded. On average, the Medicare spending in these 16 states is 20% less than in the rest of the country.
The “low-cost” states cover almost 40% of the land mass of the US but encompass only 14% of the population and only 3% of the African-American population. While they include many prominent cities, there are no major urban centers with the dense zones of poverty, as are found in Chicago, Los Angeles and New York. Nor are there broad bands of poverty, as are found in Louisiana, Mississippi, Alabama and southern Texas. Yet it is in “poverty ghettos” and broad “poverty regions” that health status is poorest and health care spending is greatest.
We must not confuse the added costs of caring for the poor with inefficiency in health care. The greatest “inefficiency” is poverty. The US will never slow the growth of health care spending unless it addresses the special needs of its most disadvantaged citizens. Health care reform should assist the hospitals and physicians who care for them. Unfortunately, a number of sections of the current bills do just the opposite.
Hospital readmissions. Section 3025 of the Senate bill (Hospital Readmissions Reduction Program) and its companion Section 1151 of the House bill (Reducing Potentially Preventable Hospital Readmissions) would penalize hospitals that have higher rates of readmissions. While increased rates may reflect substandard care in some hospitals, the more common reason for higher rates is more patients who have complex diseases processes and little social support, most of whom are poor. Indeed, when fully adjusted for severity of disease, most inter-hospital differences in readmission rates disappear.
Value and efficiency. Because providers in counties where poverty is prevalent have higher per-beneficiary spending, they would be classified as “inefficient” under Section 1123 of the House bill (Payments for Efficient Areas), while providers in the 20% of counties that have the lowest Medicare expenditures would receive a 5% bonus. In like manner, Section 3001 of the Senate bill (Hospital Value-Based Purchasing Program) would reward hospitals that have lower per-beneficiary costs for certain defined conditions (acute MI, congestive health failure, pneumonia, etc.), although it is known that expenditures for such conditions are much greater among low-income patients. I am hopeful that the Senate bill will not include the Finance Committee’s call for penalties for physicians whose resource use is in the highest decile, which would mainly affect those whose practices include poor patients with multiple comorbidities.
IOM study of geographic variation. The same logic pattern that has been applied to readmission policy and to “value-based purchasing” exists in Sections 1159 and 1160 of the House bill, which instructs the Institute of Medicine to develop payment policies based on geographic differences in health care, with the assumption that differences in the Dartmouth Atlas are relevant to cost containment. Yet MedPAC has shown that, even without adjusting for income, much of the variation disappears with adjustment for health status. But even though the bill instructs the IOM to consider income and other social determinants, there are no standards that can be applied nationally to adjust adequately for these factors. On the other hand, there are partial remedies for their effects, such as the wider use of interpreters and transitional care coordinators, as Section 1151(8) of the House bill proposes to support.
Efficiency and value are important goals, but variation in their geographic distribution is principally a reflection of variation in poverty and the prevalence of disease. That should not be a surprise. We all know that poverty varies geographically, and we know that the care of the poor is expensive. If health care costs are to be constrained, it must be through addressing the needs of low-income patients; not through penalizing the providers who care for them.

It seems like a overly simplistic way to balence medicare funds. In addition the so- called “DISH” (disproportionate share funds) will likely be cut to the public institutions in large cities, further tearing apart the “safety net.” A well funded single payor system would provide the most care for the least cost.