Academic Medical Centers and the Poor
In a recent Health Affairs blog, Wennberg and Brownlee lamented that op-eds, blogs, letters to members of Congress, broadsides in the press and now a report from the American Hospital Association decry the Dartmouth Atlas as a lot of “malarkey.” Once again they tried to defend their work by proving that race and poverty don’t matter, but they do. Even the “impartial” introduction by the editor of Health Affairs, a member of Dartmouth’s Board, couldn’t save the day: “Wennberg and Brownlee rebut claims that variations among academic medical centers are due to differences in patient income, race, and health status.” Wrong, again! That’s exactly what variations are due to.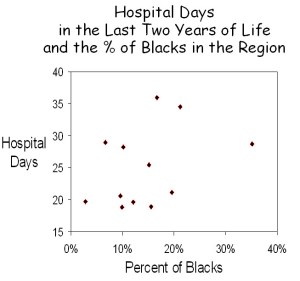
Black is not a measure of poverty. In the obtuse reasoning that characterizes the Dartmouth group, Wennberg and Brownlee’s first argument was that, although blacks utilized approximately 1/3 more care than non-blacks, the amount of care received during the last two years of life was greater in some communities than others for both black and non-black patients, and it didn’t correlate with how many blacks there were (see figure below). They concluded that “race and poverty do affect utilization. Where patients get their care matters far more than the size of their income or the color of their skin.”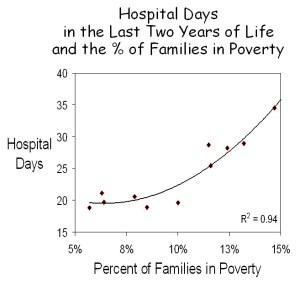
The problem is that income, which is the strongest correlate of health care utilization, was not measured, and the only skin color that was measured was black, which is not a proxy for income. In fact, in many of the communities studied, the ethnic groups with the greatest poverty were Latino or Asian.
To directly examine income, Census Bureau data on family poverty were obtained for each of the communities Wennberg and Brownlee studied, and these data were plotted against their measures of the number of hospital days used in each community. A very strong correlation was observed (R2 = 0.94), and like previous examinations of the relationship between income and utilization, it best fit a 2nd order polynomial. The answer is clear. Poverty explains a great deal about the differences in health care utilization in various communities.
Dual eligibility is not a measure of poverty. Wennberg and Brownlee next assessed the potential role of poverty in a large group of academic medical centers. To do this, they examined the relationship between the number of hospital days used by Medicare beneficiaries during the last six months of life and the percent of patients in each hospital who were dually eligible for both Medicare and Medicaid, assuming that dual eligibility is a valid proxy for poverty. They found no relationship, which led them to conclude that poverty played no role. However, their fundamental assumption was incorrect. Although dual eligibles are poor, dual eligiblility is not a proxy for poverty, as is evident in the figure below.
Dual eligibles span a diverse array of income and disabilities. They tend to be in poorer health and, although they constitute fewer than 20% of enrollees, they consume more than 30% of resources. Under federal law, state Medicaid programs must cover elderly individuals who receive Supplemental Security Income (SSI) and disabled non-elderly individuals who meet specific and income requirements, although certain states are permitted to establish more restrictive criteria and all states may extend Medicaid coverage to broader groups of elderly and disabled. Income eligibility ranges from as low as 75% of the federal poverty level in some states to > 200% in others. Approximately one-third of dual eligibles are non-elderly patients with disabilities, including end stage renal disease (ESRD). Overall, the non-elderly disabled account for 15% of Medicare beneficiaries, but the percent varies two-fold among states. Together with poor elderly who meet the income eligibility criteria, 21% of Medicare beneficiaries are dually eligible, but this number varies from about 12% in some states to more than 30% in others.
Because of differences in eligibility and in the prevalence of disability, there is little uniformity in the characteristics of dual eligibles in the various states. Moreover, as shown in the illustration above, there is no relationship between the percent of dual eligibles in a state and the percent of seniors who are at the poverty level. Wennberg and Brownlee incorrectly assumed that dual eligiblility is a proxy for poverty. It is not. The lack of a relationship between the percent of beneficiaries who are dual eligible and overall health care utilization says nothing about poverty. Rather, the direct relationship between poverty and utilization in the example above and countless others speaks volumes.
Poverty is a major factor in Medicare spending. In summarizing their remarks, Wennberg and Brownlee state that “a recent study published in the New England Journal of Medicine by some of our colleagues found that poverty and race had virtually no impact on utilization.” What this study actually showed was a strong relationship between poorer health status, greater spending and higher mortality, and it demonstrated a strong relationship between lower income and higher Medicare spending (figure below). In fact, if health care spending for all Medicare beneficiaries were at the same level as for those with annual incomes above $25,000, overall Medicare spending would be 34% less.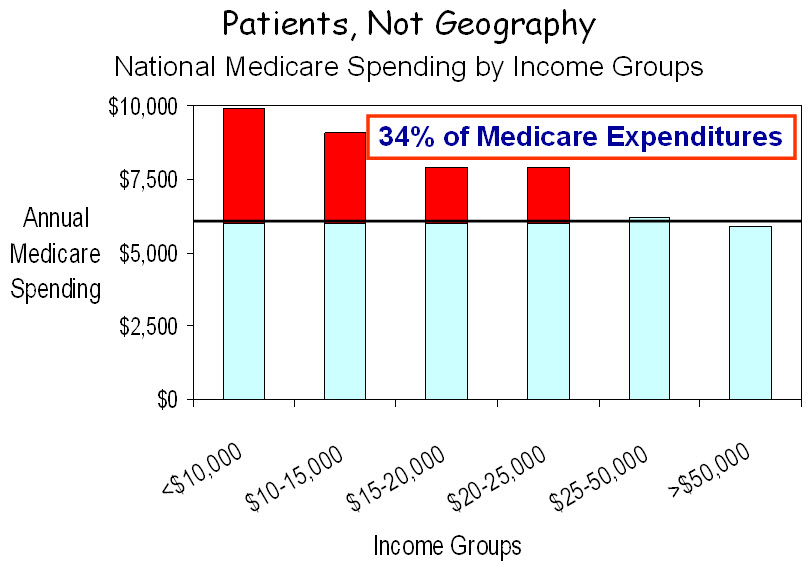 So how does one account for the statement that poverty and race don’t matter? Their Dartmouth colleagues left the real data behind and retreated into their mythical world of “quintiles,” in which the nation’s hospital referral regions are grouped into five uqintiles based on their levels of Medicare spending. This brings together disparate geographic areas which, when aggregated and averaged, all regress to the mean, and nothing is different. It’s this same shell game that gave us the “30% solution,” but the shells have been turned over, and we now know that nothing is there. Thankfully, the poor have won. Poverty matters.
So how does one account for the statement that poverty and race don’t matter? Their Dartmouth colleagues left the real data behind and retreated into their mythical world of “quintiles,” in which the nation’s hospital referral regions are grouped into five uqintiles based on their levels of Medicare spending. This brings together disparate geographic areas which, when aggregated and averaged, all regress to the mean, and nothing is different. It’s this same shell game that gave us the “30% solution,” but the shells have been turned over, and we now know that nothing is there. Thankfully, the poor have won. Poverty matters.
A challenge to Dartmouth. Wennberg and Brownlee ended their essay by pointing out that, “as guardians of the scientific basis of medical practice, academic medical centers have a special responsibility to understand why they treat similar patients differently.” Well, from everything I know, and from the vast and growing literature that supports it, the major reason for these differences is that their patients are different. This doesn’t mean that hospitals and physicians shouldn’t look for better ways to practice, even if they all practice the same. But it does mean that the differences that Wennberg and associates measure are principally related to poverty and other social determinants of disease. I would turn the challenge around: as self-proclaimed guardians of regional variation, it’s time for the Dartmouth group to stop spreading malarkey. They have a moral responsibility to do so.

Gosh, when I stare at your (untitled and only-partially-explained) second graph, I am pretty sure that a regression line would have a fairly strong positive value. You drew a line in the first graph (…even gave us an R-squared…). Let’s see you do it in the second one too.
The correlation coefficient of the regression in the other graph (Percent of Blacks vs. Hospital Days) approaches zero (R2 = 0.149). In other words, there is no significant relationship between the percent of the population in a community that is black and the amount of health care utilized. In contrast, the correlation coefficient relating the Percent of Families in Poverty to Hospital Days is extraordinarily strong (R2 = 0.935). Poverty is a very strong determinant of utilization.